Category Archives: Situational
Two Hours for a Shower—And a Lifetime of Love
Today it took two hours to help my wife, take a shower in our own home.
Two hours of lifting and moving, of prepping and adjusting.
Unhooking her IV.
Unwrapping layers of dressings and wound care.
Lining the shower with towels and placing the chair just right.
Washing her hair, combing it gently.
Finding clothes that work for a body in pain.
Changing the linens, warming the room, preparing her toothbrush—preloaded with toothpaste because her hands don’t work anymore.
Two hours of effort.
For 30 minutes of normalcy.
For 10 minutes of comfort.
For one more moment of feeling clean and human.
And then back to bed, with the “bear hugger” blowing warm air to keep her body from freezing. Her body can’t regulate temperature anymore.
She smiled when it was over.
But she’s tired.
I’m tired.
And tomorrow… she faces her third surgery in just 60 days.
We had held on to hope that she could go on the family trip to Japan—something she’s been dreaming of for a year. But this new surgery means she’ll stay behind, once again watching life from the sidelines of recovery.
That’s what cancer does. That’s what infection does. That’s what caregiving is.
It takes things—quietly, relentlessly.
It takes time, energy, tears, sleep, plans, dreams, vacations, strength.
But we keep giving. Because love gives.
I won’t give up hope.
Not today.
Not tomorrow.
Not on her.
She’s still here. Still smiling through it. Still fighting. Still loving us in her own quiet way.
So we’ll keep going.
One day at a time.
One shower at a time.
One breath at a time.
Because this is what love looks like when it’s on the battlefield.
The Power of Presence: How to Support Caregivers
When someone you love is gravely ill or bedridden, the world becomes very small. The walls of the home close in. Time slows. Days blur together. Both the person being cared for—and the caregiver—begin to live in a kind of suspended animation, where joy, spontaneity, and connection are replaced by routine, worry, and waiting.
People often ask, “What can I do?”
And it’s a sincere question. They want to help. So they send flowers. Cards. Food. Gift cards. And all of those are kind gestures. All of them are appreciated.
But if you really want to help a caregiver—and the person they’re caring for—be present. Show up.
Caregiving is not just physically exhausting. It’s emotionally isolating. The one who is ill is often trapped in their body, in their symptoms, in a bed they can’t escape. The caregiver, meanwhile, is trapped in responsibility, routine, and quiet desperation.
Isolation is the great thief.
It steals joy, perspective, and sometimes even hope. But when someone walks through the door just to be there, everything changes—even if only for a little while.
Here’s what you may not see:
When visitors come over, something shifts.
The house feels lighter.
The person being cared for suddenly wants to sit up straighter, to smile, to tell stories—even if they can’t move or speak much.
The caregiver may finally exhale, just a little.
You don’t need to bring anything. Just your presence. A shared moment. A hand held. A joke told. A prayer whispered.
It’s not about what you do. It’s about that you came.
We often overcomplicate compassion. We think we need the “right” thing, the perfect timing, or something polished and proper.
But love isn’t complicated.
Compassion shows up unannounced and says, “I’m here.”
It’s the ministry of presence.
So, if you’re wondering how to help:
- Visit. Even 15 minutes can be sacred.
- Sit. Watch a show, listen to music, share a memory.
- Talk. About something—anything—besides illness.
- Listen. Sometimes just being a witness to the struggle is a gift.
- Stay connected. Don’t let their world shrink without a fight.
Because at the end of the day, love looks like presence. And presence heals in ways medicine can’t.

AI Can’t Care – Why Human Trust Still Wins in a Tech-Driven World
In a world that feels increasingly automated, one thing is becoming clearer every day: people still crave connection. Especially when they’re hurting. Especially when they’re trying to navigate something as emotional and complex as the VA disability claims process.
At LOUJSWZ INC, we embrace technology. We use AI to make our work more efficient, more accurate. But AI is not our product. Our product is trust. And there isn’t a line of code out there that can replicate that.
I recently sat down with a fellow veteran who shared how rushed his transition was and how unsure he felt even after submitting his claim. He used the free services available to him—VFW, county VSO, mobile VA outreach—and still felt like something might have been missed. And you know what? He’s not alone. That “what did I forget?” feeling is far too common.
There are tools now that can read disability guides and recommend conditions. They’re fast. They’re free. But they don’t know how to look you in the eye and ask, “What really hurts?” They don’t hear the pause in your voice or notice the symptoms you forgot to say out loud. They don’t walk your journey. I do. I have lived it.
Porter’s Five Forces tells us that AI is shaking every industry—lowering barriers, increasing buyer power, and making substitutes more accessible. But it also tells us something else: the key to success in a competitive landscape is differentiation.
LOUJSWZ isn’t just another support service. We’re your battle buddy through bureaucracy. We know the system, yes—but more importantly, we know you. And we’re here to make sure you get what you’ve earned. No shortcuts. No automated empathy. Just people helping people, with the support of the best tools available—not the replacement of them.
Because at the end of the day, AI may shape strategy, but it’s still heart that shapes trust.

Understanding Anticipatory Grief as a Caregiver
I’ve spent a lifetime wearing uniforms — first in the military, then in business — but no uniform could have prepared me for the one I wear now: caregiver.
My wife is still here. She still smiles. Still laughs. Still says “I love you” with the same strength that got her through childbirth without a scream and once drove a screwdriver bit through her hand with nothing more than a calm “ouch.” But even with all that strength, I know what’s coming. And somewhere along the way, I realized I was already grieving.
It wasn’t denial that kept me from seeing it; I saw every scan, every new medication, every tear. It wasn’t anger that overwhelmed me, though I’ve certainly felt flashes of frustration — at broken systems, unanswered prayers, and my own helplessness. It was something quieter. Slower. A gradual ache of knowing that the woman I love is slipping away in pieces.
That’s what anticipatory grief is — mourning someone while they’re still alive. It’s showing up with love and purpose even as the shadows grow longer. It’s grieving not just the final goodbye, but the thousands of little ones along the way: the goodbye to traveling together, to her independence, to her baking and cooking in the kitchen.
I’ve come to understand that the five stages of grief — denial, anger, bargaining, depression, acceptance — aren’t a straight road. They’re more like a roundabout we circle again and again. And while Kübler-Ross introduced them to describe how patients face terminal illness, caregivers like me feel them too — just in advance.
Right now, I live somewhere between acceptance and heartbreak. I’ve accepted what’s coming. But each day, I still fight to create joy, dignity, and presence. We watch movies in the car so she doesn’t have to get out. We eat takeout in the bed because she cant sit at the table. I hold her hand not just in sickness, but in the holy weight of being here — now.
If you’re walking this road too, know that grief doesn’t wait for death. And love doesn’t wait for perfection. You are doing holy work, even when your hands feel empty.
Let yourself grieve. But also — let yourself love, fiercely, while there’s still time.


The Truth About Insurance Delays in Medical Equipment Access
Imagine this: your loved one has just been admitted to a rehabilitation hospital. She has limited mobility, use of only one hand, and is in critical need of a powered wheelchair to regain a sliver of independence. The medical team sees the need clearly. The rehab team jumps into action—generating a physician’s statement of need, identifying a qualified vendor, and aligning care planning around the use of this essential device.You would think the next step is straightforward—insurance approves, device is delivered, and your loved one can begin her recovery journey with dignity.
Wrong.
The insurance company’s response? “It will take a minimum of 60 days to process.” That’s 45 days after the patient is discharged—leaving her bed-bound or reliant on round-the-clock support in the meantime. If you want the device sooner, it’s available—but only if you can pay the full cost upfront, out of pocket.Luckily, I had just enough space on a credit card—$2,200—and I bought the chair myself. Within hours, it was delivered. The result? My wife, who was at risk of becoming isolated in her own home, regained some independence. We then submitted all the paperwork for reimbursement through the approved process—yes, still by fax in 2025. The insurance company now has 75 days to decide whether the benefit will be honored.And what if they do approve it? After deductibles, co-pays, and co-insurance calculations, they’ll only reimburse less than 50% of the total cost.This experience was frustrating, disheartening—and honestly, a little scary. What happens to people who don’t have a credit card? Who can’t float the cost while waiting months for reimbursement? Are they just expected to sit, lay, and suffer in silence?—The Business Rules Are Broken. Health insurance providers often tout their “support” for necessary medical equipment. But their business rules are built for denial, delay, and discouragement:Delays in processing—even with a signed medical necessity letter.Reimbursement after the fact, not timely fulfillment.Inadequate coverage—only partial payments after all the math. And yet, the market has made it possible to buy a power chair on the same day. The disconnect is glaring: it’s not a matter of availability, it’s a matter of access.
—Final Thoughts: This post isn’t about venting. It’s a call to advocate for change. Durable medical equipment (DME) is not a luxury—it’s a lifeline. Yet current insurance practices treat it like an optional convenience.If you’re a caregiver, patient, or family member going through this system, I see you.
If you’re a policymaker or insurance executive reading this, I urge you—align the policy to the people. Because right now, too many are being left behind.—If you’ve faced similar challenges or want to share resources that have helped you navigate the DME approval process, please share them in the comments. We need to amplify these stories and stand together for better healthcare access.

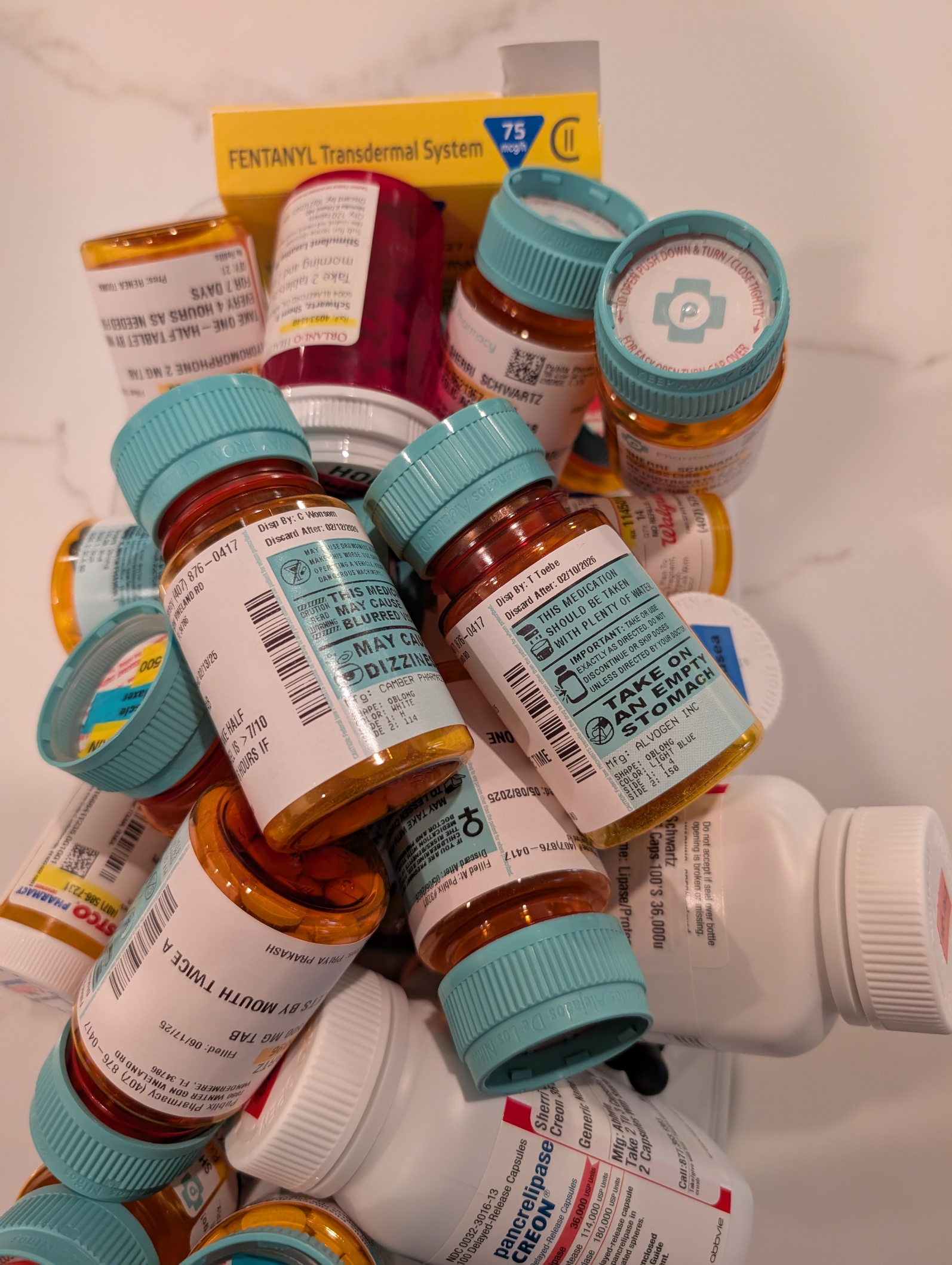
Pills, Pills, and More Pills: The Hidden Burden of Complex Caregiving
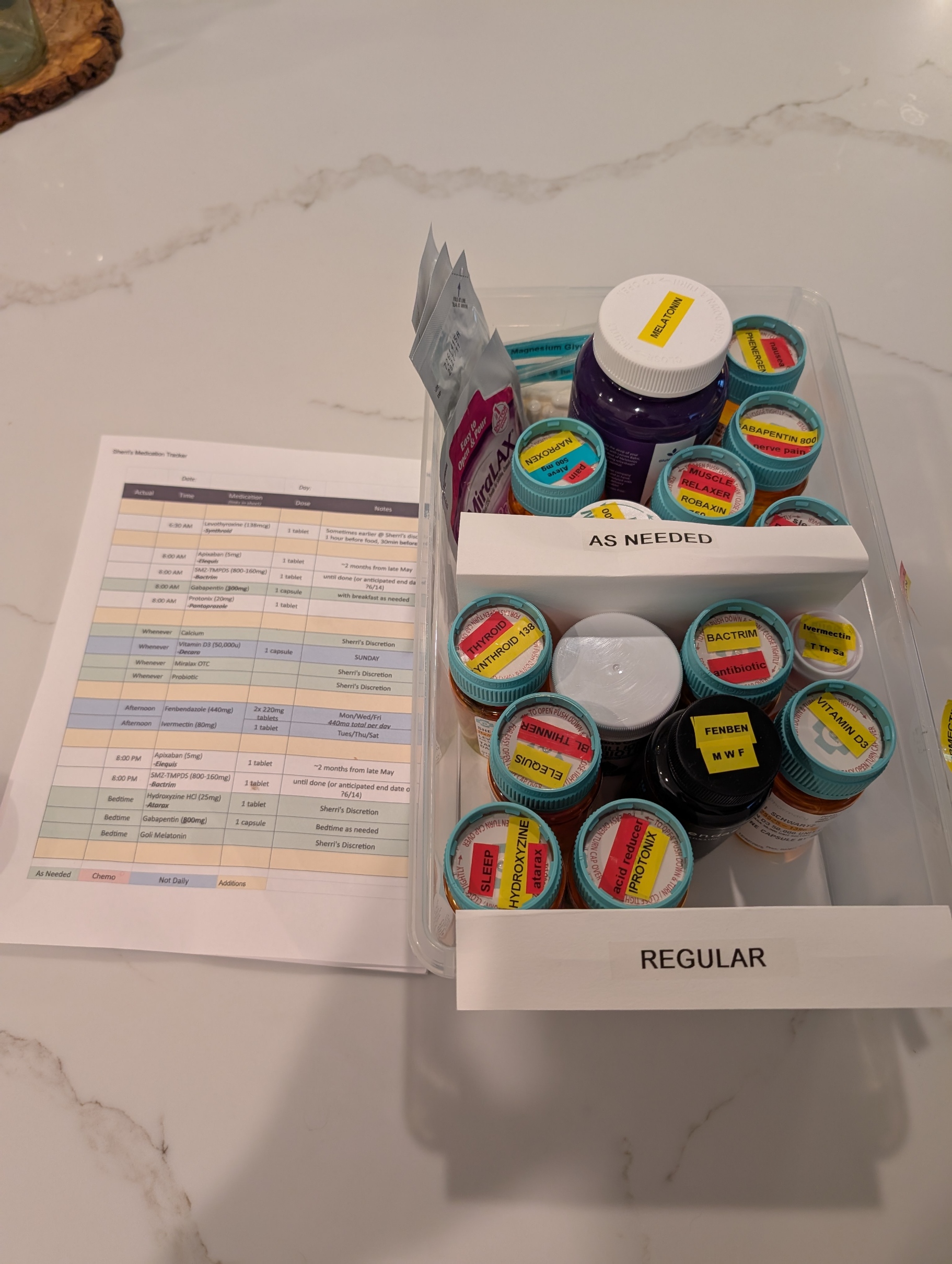
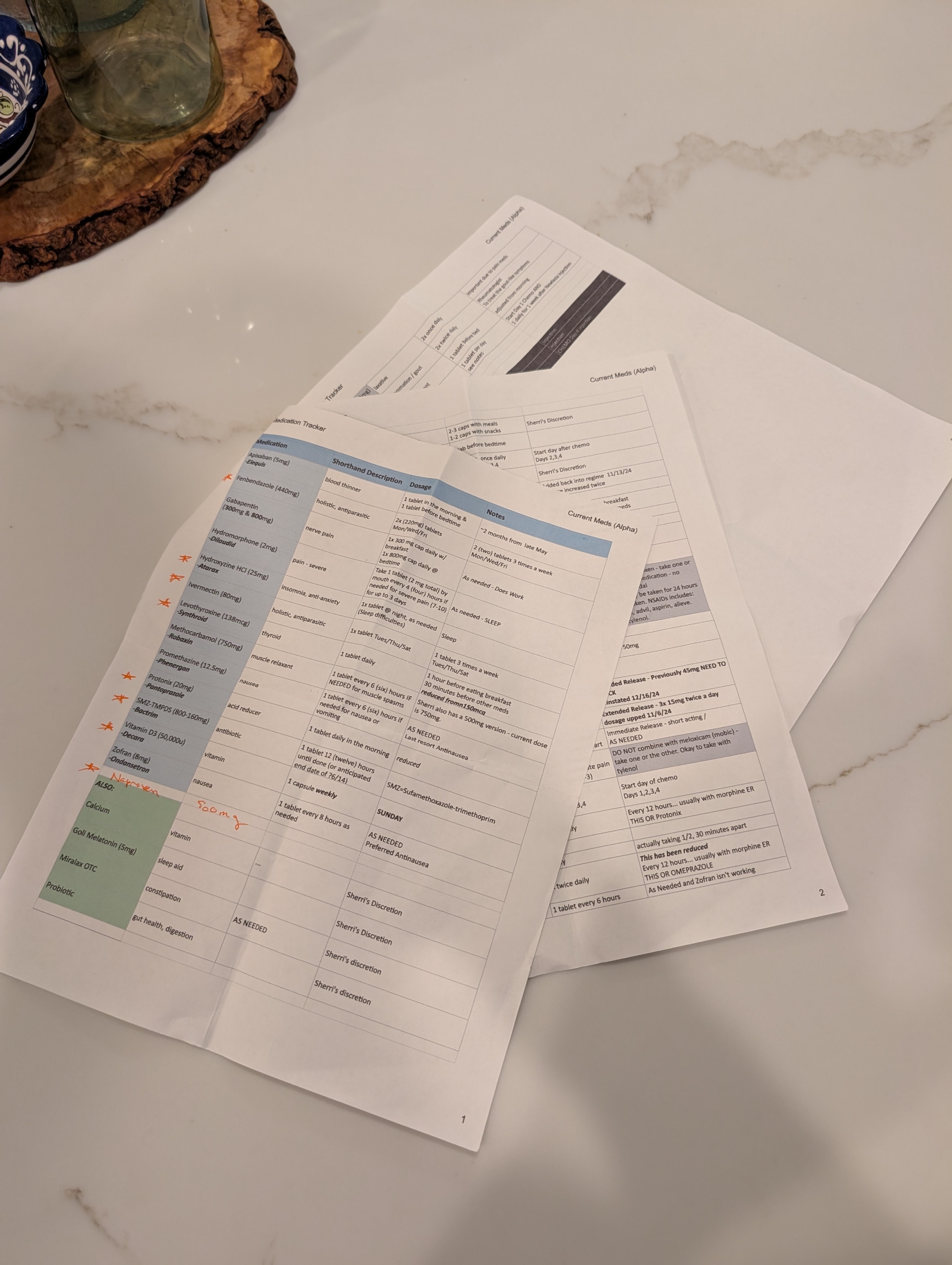
One of the most overwhelming challenges in being a caregiver to a loved one with complex health needs is managing medications. It’s not just about handing over a pillbox. It’s navigating a labyrinth of prescriptions from multiple providers—some within the same healthcare system, others outside it, and even some who are technically in the system but don’t have credentials to see each other’s records. The result? A fragmented network of well-meaning professionals relying on the patient or caregiver to connect the dots.
Every outpatient visit starts with the same question: “Are you still taking…?” And if your loved one isn’t completely lucid or you’re not fully dialed in 24/7, the answer might not be accurate. That’s when the real risk begins. Medications get missed, taken at the wrong time, or worse—interact dangerously. Even with tools like MyChart and pharmacy alerts, medication management for multi-disciplinary patients is a full-time job that demands vigilance and coordination.
Thankfully, my wife has what many don’t: an extended family care team. Her sister—a brilliant organizer—maintains a shared medication log with active and retired prescriptions. Her cousin, a provider based in California, monitors her records through MyChart and flags potential issues or treatment recommendations. Their support has been nothing short of lifesaving.
As her primary caregiver, I also leaned into my background in healthcare and team leadership. I applied principles I once used to support the care for wounded or sick soldiers returning from Iraq at Fort Moore (then Fort Benning), where we built systems but more importantly had people to prevent our service members from getting lost in the shuffle. It’s painful to see that the civilian system still struggles with the same problem.
Where is the care manager? Aren’t they the quarterback? I once asked that question myself—only to be told their panel included 250 complex cases. No human can meaningfully manage that many lives. It was a sobering reminder that “the system” is overloaded, and for those without advocates, the consequences can be tragic.
Having a palliative care physician onboard has been critical. Contrary to common perception, they don’t just deal with end-of-life care. They focus on quality of life—managing pain, coordinating care, and yes, reconciling all those pills. My wife currently has more than 10 providers involved in her care. That number doesn’t include staff, specialists, or the relentless demands of insurance approvals.
Medication management isn’t glamorous, but it’s a battlefield—and like all battlefields, it requires a team, a plan, and an unwavering commitment to the person you’re fighting for. I bring my military mindset to this mission every day. And while I can’t stop the tide of prescriptions or the systemic gaps in care, I can make sure my wife never faces them alone.


The Art of Caregiving: Strategies for Support
“You have to go for a walk. Take a hot shower. Make sure you hit the rack every night early. I mean like 2000 hours at the latest. Every day is just like the military. You’re preparing for the next day.”
That’s what my buddy—another veteran who recently lost his wife to pancreatic cancer—told me. It stuck. Not because it was profound (although it is), but because it was familiar. It’s the kind of advice you’d hear before a deployment. Only now the mission is different. It’s longer. Harder in ways I never expected. And it’s personal.
My wife Sherri is currently watching a movie in our EV, having lunch with our fur babies. It’s a simple solution to a hard problem: it spares her the pain of getting out of the car, into the electric wheelchair, into the house—only to turn around and do it all again in 35 minutes. During that time, my sister-in-law (who’s been a godsend) and I tag-teamed lunch prep, charged the chair, rotated the laundry, and coaxed our teenager into eating something besides cereal. That’s the rhythm. That’s the operation.
It’s funny how much this mirrors the military. In downtime, you prep for the next mission. That’s what caregiving is: a constant cycle of readiness. Because when your loved one is in pain, even helping them move can feel like a landmine of unintended harm. You don’t get to wing it. You plan, prep, adapt, and repeat.
And here’s the kicker: you can’t pour from an empty canteen.
My friend reminded me—like a good NCO would—that I need rest. That I need to recoup. That doing “me time” isn’t selfish; it’s strategic. And yet it’s one of the hardest things to do. How do you step away when the person you love is hurting? But if you don’t, you break down. And when you’re broken, you’re no good to them.
For me, that “me time” is Orange Theory Fitness. It’s more than a workout—it’s my decompression chamber. The people there know my story. They don’t flinch when I show up in a weird mood or vent a little too hard. They get it. It’s a release valve.
But caregiving can’t be done alone. It requires an extended care circle, and let me tell you—building that after the crisis hits is like trying to patch the roof in a thunderstorm. As JFK said, “Fix the roof when the sun is shining.” He wasn’t wrong. Having my sister-in-law here has changed everything. And when she’s not, our neighborhood friends step up in ways that humble me. They’re part of the circle now. I’ve learned that asking for help doesn’t make you weak—it lets people love you in real, tangible ways.
There’s something beautiful about how people show up when you let them. It reaffirms your faith in humanity, even on the hardest days. And if you’re lucky—like I am—you see that caregiving, as hard as it is, is also a sacred kind of service. One where love, not rank, leads the charge.
So here’s what I’ll leave you with:
Build your circle when the skies are clear.
Rest like it’s your responsibility—because it is.
And never underestimate the power of kindness, sweat equity, and a hot shower.
Because when it’s raining, all of that matters more than you’ll ever know.

“Holding On: A Caregiver’s Reflection on Love, Loss, and Living in the Now”
My wife came home today.
After nearly a month that felt like a lifetime—through the emergency room, the operating room, recovery, and finally a rehabilitation hospital—she is back, sitting at the kitchen table with our daughter and her sister. They’re talking about summer camp. It sounds so normal. It looks so beautiful. And yet, nothing about this is normal.
She has four broken bones—fragile from cancer that has metastasized into her bones. She cries now, often. More than I’ve ever seen in all the years we’ve been together. Her voice is quiet. Barely audible sometimes. She has only her hands now to guide her through the world, needing an automated wheelchair that still hasn’t arrived because insurance bureaucracy doesn’t move at the speed of human need.
I was ready to buy one. But she said, “No. We’ll wait.” And so we do. Because this is her journey. And while everything in me wants to fix it—to make it easier, faster, better—I know what she needs most is for me to walk beside her, not ahead.
This is not my first time walking this path. I’ve been here before. With my sister. With my father. But knowing the route doesn’t make it easier. It just makes the heartbreak familiar.
Yet she continues to defy the odds. She is part of the 3% who’ve made it this far. A walking miracle. A living lesson in endurance. So we stay grateful. We stay hopeful. We keep our chins up—not just for her, but for ourselves and everyone around us.
Caregiving is the quiet battlefield. You fight fatigue, frustration, and the aching helplessness of watching someone you love suffer. You become nurse, advocate, counselor, and spiritual anchor—all while trying to remember who you are.
But caregiving also sharpens your vision. You begin to see what matters.
It’s the sound of her voice, barely above a whisper, joining in a conversation at the table.
It’s the laughter that somehow still finds its way into our home.
It’s the love that survives even the most brutal storms.
We often think of time as a currency, but when you’re a caregiver, you realize it’s far more precious than money. It is sacred. It is fleeting. It is everything.
So if you’re reading this in the middle of your own storm, hold on. Don’t just wait for the clouds to pass—find the grace in the moments in between. Because even in the darkest stretches, there is light. Sometimes it’s a whisper. Sometimes it’s a smile. Sometimes it’s just sitting quietly at the kitchen table with the ones you love.
Hold onto that.
The Joy of Collecting: Finding Meaning in Everyday Treasures
I’ve always collected things—medals, pennies, shark teeth, rocks, golf balls, even tire valve caps. Some of these were intentional, others accidental. But all of them, in their own way, represent little victories and moments of peace.
Just the other night, I went on a walk after dinner, a habit more about unwinding than fitness. I came back with five golf balls. Five. That might not seem like a lot to some people, but for someone who’s spent a lifetime collecting, five of anything in one outing is a haul. It got me thinking—not about golf balls, but about collecting, and more curiously, why I do it.
Let me start with this: I’ve begun using lost golf balls as my own personal economic indicator. A kind of SWAG (scientific wild-ass guess). I know it’s a stretch, but hear me out—if people are out playing golf in the middle of the week and losing $20 sleeves of balls without a second thought, then someone out there is doing alright. I’m no fan of trickle-down economics, but the existence of a well-funded slice of the population still swinging away gives me a small sense of hope that the world hasn’t completely unraveled. Still, that’s not why I walk. I walk to escape that kind of thinking.
This post isn’t about economics. It’s about collecting.
My father used to collect pennies he found on walks. Before that, as a boy, he collected stamps. I picked up the penny habit from him, and at one point, my collection was medals—military ones. Now? It’s golf balls, and teeth from long-dead sharks. And that’s the distinction I want to make. Stamps and medals feel like hobbies. You go out, you pay money, you build your collection. But to me, collecting has always been about the hunt—the unplanned, unscheduled discovery. The moment you spot something unexpected glinting in the grass or poking out from the sand. That’s collecting.
There’s real joy in that moment—when you pause, bend down, and confirm that yes, it’s a golf ball or a shark tooth or some little artifact the world left behind. It feels like you’ve won something. Like you’re seeing what others overlook. It might sound like a stretch, but in those moments I feel capable, even special.
Turns out, there’s science to back that up. Psychologists have long studied the drive to collect. Some say it’s tied to our ancestral instincts—early humans were gatherers, after all. Others say collecting brings order to chaos, structure to a fast-moving world. According to researchers, collecting can also provide a sense of control, personal identity, even legacy. But more than that, when we find something—especially something unexpected—our brain releases a hit of dopamine. The same reward chemical that fires when we eat good food, laugh, or fall in love. So yes, spotting a golf ball in the grass isn’t just coincidence—it’s chemically rewarding. No wonder I keep looking.
In those moments, I’m not thinking about work, or stress, or the headlines. I’m just walking. And collecting. And somehow, connecting to the people who came before me—my dad and his pennies, the long-lost owner of the golf ball, even the shark whose tooth found its way into my palm.
Collecting, for me, isn’t about things. It’s about finding meaning in the everyday. It’s about knowing that even in a world spinning out of control, there are still small, lost treasures waiting to be found.

The Life-Saving Power of Blood Donation
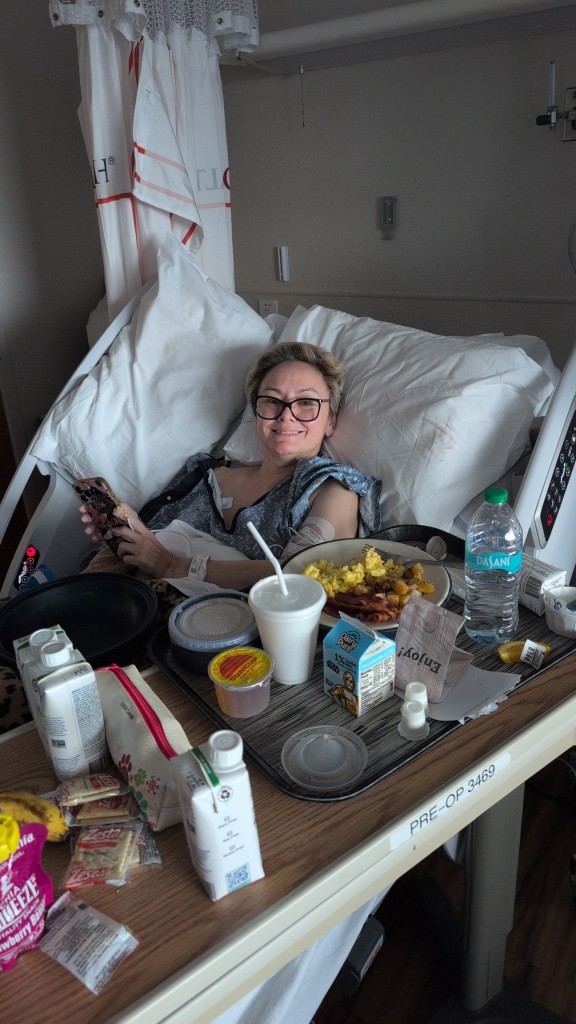





There are moments in life that transcend coincidence—moments that remind us of the deep interconnection between people, acts of service, and the enduring power of compassion. My wife and I recently experienced one of those moments firsthand.For years, we’ve both been regular blood donors. It was never about recognition or reward—it was simply the right thing to do. We believed in it. We knew that a single pint of blood could mean the difference between life and death for someone we might never meet. What we never imagined was how this quiet act of giving would one day come full circle in our own lives.Over 30 years ago, I required an emergency blood transfusion after surgery. I had been discharged from the hospital, only to collapse at home from undetected internal bleeding. As my strength faded and my consciousness waned, two pints of blood were administered, and within minutes, I felt myself come back to life. I will never forget that sensation—the sudden clarity, the renewed energy, the overwhelming gratitude for whoever had made that donation.Fast forward to the present: my wife is fighting cancer with a strength that humbles me every day. Recently, her care team determined she needed a blood transfusion. I told her what I had experienced—that maybe she, too, would feel the same miraculous lift. And she did. That night, she slept peacefully. Her color improved. Her energy returned. It was an almost immediate renewal of life.In that moment, all the years we spent donating blood felt like a sacred thread—woven into a story we could never have predicted. One act of generosity can become someone else’s lifeline. And sometimes, that “someone” is the person you love most in the world.Blood is more than a clinical fluid—it’s a vessel of hope, a symbol of our shared humanity. Donating blood is not just a medical gesture; it’s a profound act of connection. When we give, we’re not only offering a piece of ourselves—we’re becoming part of a legacy of compassion that could touch lives in ways we may never see.I encourage everyone reading this to consider becoming a donor. You may never know whose life you’ll save—but one day, that life might just be someone you love.


